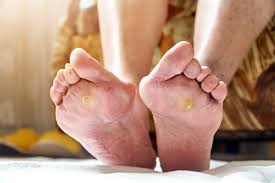
What is a diabetic foot ulcer?
Diabetic foot ulcer is a skin sore with full thickness skin loss on the foot due to neuropathic and/or vascular complications in patients with type 1 or type 2 diabetes mellitus.
Causes of diabetic foot ulcer
- Peripheral Neuropathy: High blood sugar levels can damage nerves, leading to a loss of sensation in the feet. This means injuries may go unnoticed, allowing ulcers to develop.
- Poor Circulation: Diabetes can lead to vascular disease, reducing blood flow to the feet, impairing healing and increasing infection risk.
- Foot Deformities: Conditions such as bunions, hammertoes, or Charcot foot (bone deformities) can create pressure points that lead to ulcers.
- Infections: Minor injuries or skin breakdowns can become infected, especially in individuals with compromised immune systems.
- High Blood Sugar Levels: Elevated glucose levels can impair the healing process and increase the risk of ulceration.
Risk Factors of diabetic foot ulcer
- Diabetes Duration: Longer durations of diabetes increase the risk of complications, including foot ulcers.
- Uncontrolled Blood Sugar Levels: Poorly managed diabetes raises the risk of neuropathy and poor circulation.
- Previous Foot Ulcers: A history of ulcers increases the likelihood of future occurrences.
- Smoking: Tobacco use impairs circulation and healing, exacerbating foot problems.
- Obesity: Excess weight can increase pressure on the feet and exacerbate foot deformities.
- Inadequate Foot Care: Lack of proper foot hygiene and care can lead to unnoticed injuries and infections.
Symptoms of diabetic foot ulcer
- Sores or Wounds: Open sores on the foot, particularly on pressure points, are the most obvious symptom.
- Redness and Swelling: Surrounding tissue may become red and swollen due to inflammation or infection.
- Pain or Discomfort: Some individuals may feel pain, although neuropathy can mask this sensation.
- Foul Odour: Infected ulcers may emit a foul smell.
- Drainage: Pus or fluid may leak from the ulcer, indicating infection.
How is diabetic foot ulcer diagnosed?
Diabetic foot ulcer is a clinical diagnosis of a painless foot ulcer in a patient with a long history of poorly controlled diabetes mellitus.
Investigations may include:
- Swabs for secondary infection
- X-rays for bone involvement
- Angiography.
What is the treatment for diabetic foot ulcer?
Prevention of diabetic foot ulcer
- Optimise diabetes control to reduce neuropathic and vascular complications
- Smoking cessation
- Regular examination of the at-risk foot, and careful toenail trimming
- Prompt treatment of non-ulcerative conditions such as tinea pedis or cracked heels
- Appropriate footwear — properly fitting soft shoes or made-to-measure insoles
- Exercise and physiotherapy
- Education of patient, family, and healthcare providers
General measures
- Multidisciplinary care — may include endocrinologist, podiatrist, diabetes education nurse, wound care nurse, neurologist, vascular surgeon, and/or orthopaedic surgeon
- Pressure reduction — appropriate footwear, crutches
- Control of blood sugar levels
- Prevention of secondary infection
Specific measures
- Treatment of secondary infection
- Ulcer debridement
- Dressings
- Adjuvant therapies — negative pressure wound therapy, ulcer excision and grafting, topical or hyperbaric oxygen, human growth factors, and/or amputation
What are the complications of diabetic foot ulcer?
- Infection: Untreated ulcers can lead to serious infections, potentially resulting in cellulitis or osteomyelitis (bone infection).
- Gangrene: Severe infections can lead to tissue death, requiring amputation of the affected toe, foot, or even part of the leg.
- Chronic Pain: Some individuals may experience long-term pain or discomfort from foot issues.
- Loss of Mobility: Severe complications may result in decreased mobility, impacting quality of life.
What is the Preventions for diabetic foot ulcer?
The best treatment for diabetic ulcers is prevention. To help manage foot health, people should regularly check their feet and attend appointments with their podiatrist. Depending on certain risk factors, a doctor may recommend regular foot examinations every 1–6 months.
Tips to help prevent ulcers Trusted Source include:
- keeping the feet clean, moisturized, and dry
- wearing shoes that fit correctly
- checking the skin daily for any blisters, cracks, cuts, ingrown toenails, and other minor injuries
- keeping sugar levels within target ranges
- not walking barefoot
- seeing a podiatrist for any injuries
- quitting smoking, if applicable
Conclusion
Diabetic foot ulcers pose a major problem for people with diabetes and can result in severe health issues without proper care. It’s crucial to know what causes them how to spot them, and ways to treat them if you have diabetes. Taking good care of your feet keeping your blood sugar in check, and seeing a doctor can help stop foot ulcers from happening or getting worse. If you think you might have a foot ulcer or are having any foot troubles, don’t wait to get medical help.